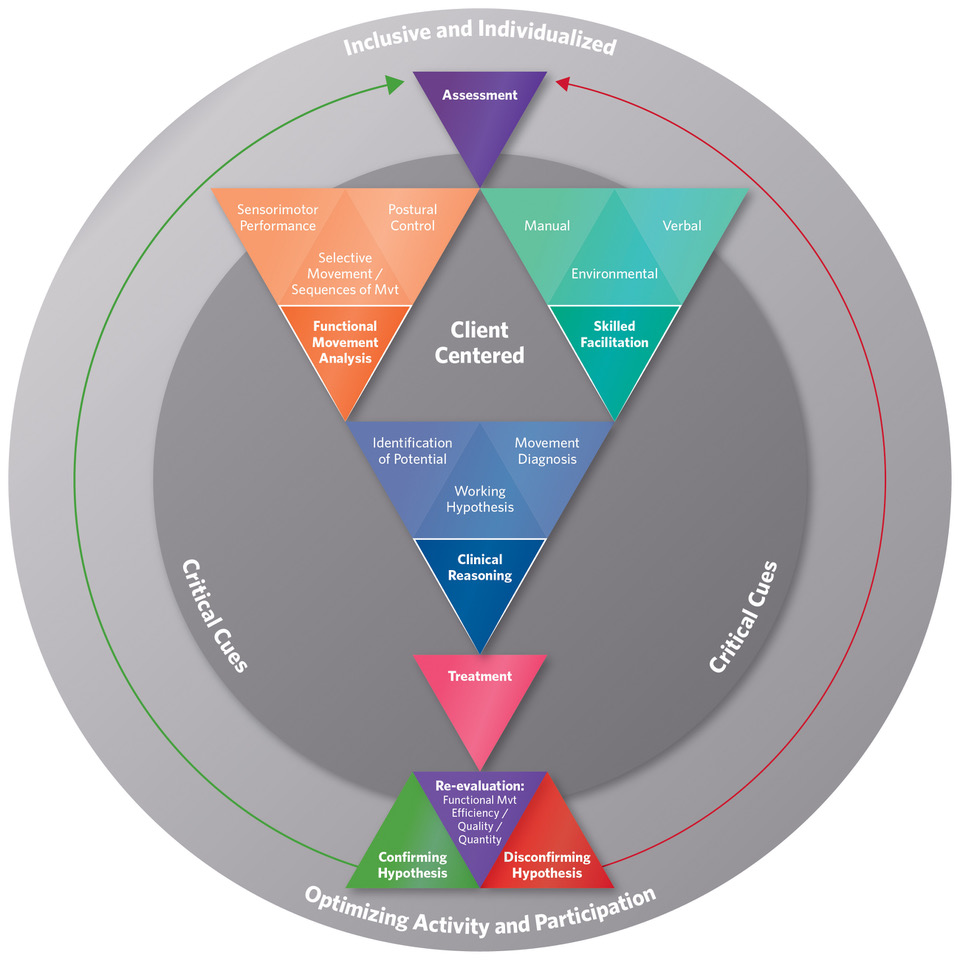
The Model of Bobath Clinical Practice. Michielsen M, Vaughan-Graham J, Holland A, Magri A, Suzuki M. (2017). The Bobath concept – a model to illustrate clinical practice. Disability and Rehabilitation, 7, 1-13. Figure 2, page 3)
Introduction
A clearly defined model of Bobath clinical practice has been lacking in the current evidence base. This creates confusion as to what actually the Bobath concept is in clinical practice and leads to misinterpretation and misrepresentation within the literature.
The IBITA Education Committee commenced work on developing a Model of Bobath Clinical Practice under the leadership of Susan Ryerson in 2008. This model is the clinical parallel to the publication by Vaughan-Graham et al., (2009) which outlines the theoretical underpinning of a contemporary Bobath concept.
The aim of this model is to identify what is unique to the Bobath concept in terms of contemporary neurorehabilitation. The model is not a model of ‘best practice’ and therefore does not seek to include all of the basic requirements of assessment that every therapist would routinely undertake.
The model seeks to identify the following:
- Aspects of cinical practice that are a focus of the Bobath concept
- Relationships that are unique to the Bobath concept
- Provision of a framework for research
The Education Committee has presented successive versions of this model for review and discussion by the IBITA membership, solicited feedback and made subsequent revisions.
The model was published in the journal of Disability and Rehabilitation Michielsen M, Vaughan-Graham J, Holland A, Magri A, Suzuki M (2017): The Bobath concept – A model to illustrate clinical practice. Dec 17:1-13. doi: 10.1080/09638288.2017.1417496. [Epub ahead of print]
The article describes the clinical application of the Bobath concept in terms of the integration of posture and movement with respect to the quality of task performance, applying the Model of Bobath Clinical Practice.
Implications for rehabilitation include:
- The Model of Bobath Cinical Practice provides a framework identifying the unique aspects of the Bobath-concept.
- The Model of Bobath Clinical Practice provides the basis for a common understanding with respect to Bobath clinical practice, education, and research.
- The clinical application of the Bobath-concept highlights the integration of posture and movement with respect to the quality of task performance.
- Facilitation, a key aspect of Bobath clinical practice, positively affects motor control, and perception.
Description of Terms
Inclusive and individualised
The Bobath concept can be applied to individuals of all ages and all degrees of physical and functional disability (Raine 2006; Raine 2007; International Bobath Instructors Training Association 2008). Bobath interventions are client centred, complex, multi-dimensional, response- based and reflective (Cott et al. 2011).
Optimising activity and participation
The Bobath concept is congruent with the ICF, recognizing that optimising activity and participation requires an understanding of the relationship between the client’s health condition, personal factors, environmental and the individual contexts enabling the identification of meaningful functional goals as an aspect of the intervention plan (Vaughan-Graham et al. 2009; WHO 2002).
Functional movement analysis
Functional movement analysis is a descriptive process of human movement of either an aspect of a task and/or the performance of a task within daily life. The Bobath concept considers how a task is accomplished. This involves detailed observational analysis of sequences of movement during task performance enabling the Bobath clinician to determine how the movement differs from typical motor behaviour, including analysis of the compensatory strategies utilized. Task analysis comprises both visual and tactile components, whereby the therapeutic handling skill of the Bobath clinician informs the analysis and contributes to the clinical reasoning process. The Bobath concept bases task analysis and intervention on an understanding of the integral relationship between postural control and task performance which requires selective movement control for the production of coordinated sequences of movement (Vaughan-Graham et al. 2009). The Bobath concept considers not only task completion / assistance required, but also the nature of the performance of the task i.e. the quality, and efficiency of task performance is an integral aspect of assessment and treatment (Levin & Panturin 2011).
Skilled facilitation
The Bobath concept has always, and continues to use facilitation as a unique aspect of intervention. Facilitation refers to making the task possible through skilled manual and environmental changes, as well as the use of verbal cues. Facilitation is a skill dependent upon the integration of the Bobath clinician’s stereognostic capacity (the ability to interpret, integrate and execute therapeutic handling), movement control, and extensive theoretical and professional practice knowledge base.
Critical cues
Critical cues are aspects of the clinical presentation that the Bobath clinician identifies as significant and thus influence the clinical reasoning process. Critical cues may include aspects of alignment, movement patterns, musculoskeletal issues, specific responses to facilitation or lack of, client preferences, comorbidities, cognitive/perceptual strengths or weaknesses.
Clinical Reasoning
The Bobath clinician reflects on all information gathered and begins to develop a working hypothesis, or hypotheses, to frame the clinical presentation. Through this process the Bobath clinician gathers relevant critical cues with respect to postural control, selective movement, sequences of movement, and task performance. This gathering of information directs further movement analysis, context-based to the individual client. The clinical reasoning process requires the systematic gathering of information which is dependent upon the individual clinician’s theoretical knowledge base, professional practice knowledge and skill level.
Movement diagnosis
The Bobath clinician, whilst acknowledging the client’s health condition and relevant restrictions, provides intervention based upon a movement diagnosis and thus a working hypothesis. The movement diagnosis is a compilation of the significant aspects of the functional movement analyses/characteristics of the individual clinical presentation. Thus the Bobath clinician does not treat “the neurological condition”, but treats the individual impact of the neurological condition on the client from movement, perceptual and cognitive perspectives.
Identification of potential
The Bobath concept has always utilized the inherent plasticity within the system to the positive benefit of the client. The Bobath clinician seeks to do this from the perspective of recovery, rather than compensation (Levin 2009). The Bobath clinician recognises the potential of the client for positive functional recovery, underpinned by the principles of neuromuscular plasticity and motor learning, whilst recognizing the limitation of the neurological deficit. The Bobath clinician seeks to do this from the perspective of sensorimotor recovery, whilst minimizing compensation and atypical motor behavior. Functional movement analysis from the perspective of the Bobath concept recognises that recovery based on compensatory movement may limit the restoration of typical motor behavior (Levin & Panturin 2011); (Michaelsen et al. 2006).
Working hypothesis
The Bobath clinician, based on the movement diagnosis and identification of potential, will select an appropriate working hypothesis. This will guide the intervention plan with respect to postural control, task performance, selective movement and sequences of movement. The Bobath clinician reflects ‘on-action’, and ‘in-action’, thus revising the working hypothesis / hypotheses and movement diagnosis in an iterative process, dependent upon the client’s response to intervention (Schon 1983).
Treatment
Treatment intervention aims to optimise activity, participation and subsequent subjective quality of life. Interpretation of critical cues is a skillful, logical and systematic step-by-step progression, individual to the client to achieve efficient muscle activation for success in a given activity or task. Treatment should provide a rich source of afferent information to maintain, restore or update body schema such that feed-forward postural control and movement control is optimised (i.e. skilled facilitation).
Evaluation of movement efficiency, quality and quantity
The Bobath clinician has specific expectations of how postural control, task performance, selective movement and/or sequences of movement will change based on the intervention. This is the result of a complex interaction of action, perceptual and cognitive systems. This is a critically reflective process to confirm or disconfirm the hypothesis and thus deepens the Bobath clinician’s professional practice experience and professional practice knowledge. The significance of positive changes with respect to the intervention is an indication of the correctness of the hypothesis, the potential of the client and the skill of the Bobath clinician. The Bobath clinician evaluates intervention from the perspective of quality / efficiency of the movement or task, i.e. formatively / diagnostically within a treatment session, as well as from a quantitative perspective, using validated, relevant outcome and objective measures which demonstrate meaningful and significant change (Levin & Panturin 2011).
References
- Cott, C., Vaughan-Graham, J. & Brunton, K. (2011). When will the evidence catch up with clinical practice. Letter to the Editor. Physiotherapy Canada, 63(3), 387-390.
- International Bobath Instructors Training Association. (2008). Theoretical Assumptions and Clinical Practice Retrieved October 29, 2012
- Michielsen M, Vaughan-Graham J, Holland A, Magri A, Suzuki M. (2017). The Bobath concept – a model to illustrate clinical practice. Disability and Rehabilitation, 7, 1-13.
- Michielsen M, Vaughan-Graham J, Holland A, Magri A, Suzuki M. (2019). Responding to Comments – The Bobath concept – a model to illustrate clinical practice. Disability and Rehabilitation 41(17):2109-2110. doi: 10.1080/09638288.2019.1606946. Epub 2019 May 9.
- Raine, S. (2006). Defining the Bobath concept using the Delphi technique. Physiotherapy Research International, 11, 4-13.
- Raine, S. (2007). The current theoretical assumptions of the Bobath concept as determined by the members of BBTA. Physiotherapy Theory and Practice, 23(3), 137-152.
- Vaughan-Graham, J., Eustace, C., Brock, K., Swain, E. & Irwin-Carruthers, S. (2009). The Bobath concept in contemporary clinical practice. (Grand Rounds)(Report). Topics in Stroke Rehabilitation, 16(1), 57-68.
BITA Education Committee July 2019
MBCP teaching resources are available for members